Evaluation of Lung Sliding
The depth of ETT insertion can also be evaluated using lung POCUS. Normal lung sliding indicates aeration of the lung. The movement caused by inflation of the lung can be seen as the visceral and parietal pleura move and is called lung sliding or shimmering. As such, presence of bilateral lung sliding indicates endotracheal intubation with an ETT positioned above the carina. The absence of lung sliding suggests the lung is not being ventilated and raises suspicion for esophageal intubation. If unilateral lung sliding is seen, it can suggest mainstem intubation [18].
Lung ultrasound can be performed with the patient in the supine position, using a linear or curvilinear probe placed in the longitudinal plane on the anterior chest of the patient at the midclavicular line. This is performed on both the left and right anterior chest walls. The relevant anatomic structures for this view are the pleural line, chest wall musculature and the ribs and their acoustic shadows (Video 3)
Important limitations to using lung sliding for confirmation of ETT depth include diseases and conditions that affect the pleura and therefore lung sliding on POCUS. This includes pneumothorax, pleural disease and contralateral lung sliding despite mainstem intubation because of retrograde air movement.
Video 3. Lung ultrasound video performed using a linear probe placed in the longitudinal plan on the anterior chest of the patient at the midclavicular line demonstrating pleural line with normal sliding.
Video 4. Lung ultrasound video performed using a linear probe placed in the longitudinal plane on the anterior chest of the patient at the midclavicular line demonstrating absent lung sliding
M-Mode can also be used to confirm the presence of lung sliding. In a normal lung where lung sliding is present, the “sand on the beach” or “seashore” sign can be observed (Figure 6A). Conversely, absence of lung sliding will create the “stratosphere” or “barcode” sign (6B).
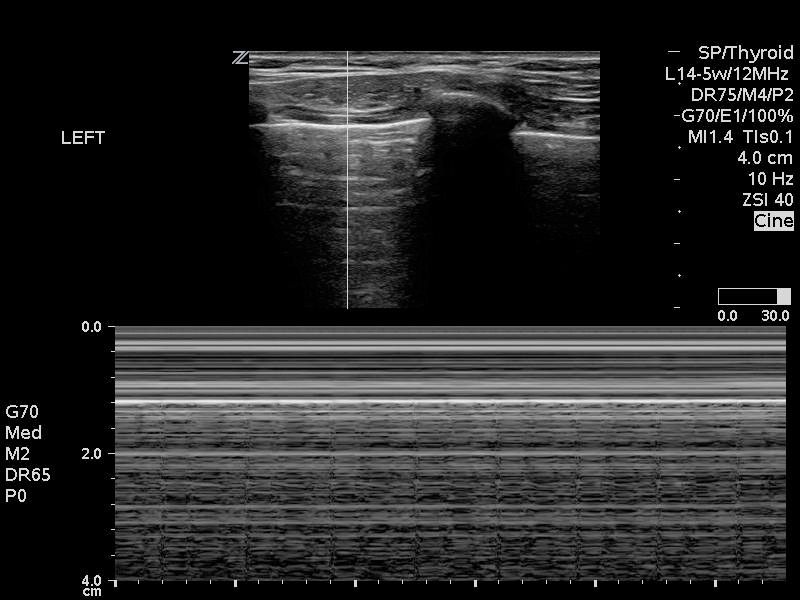
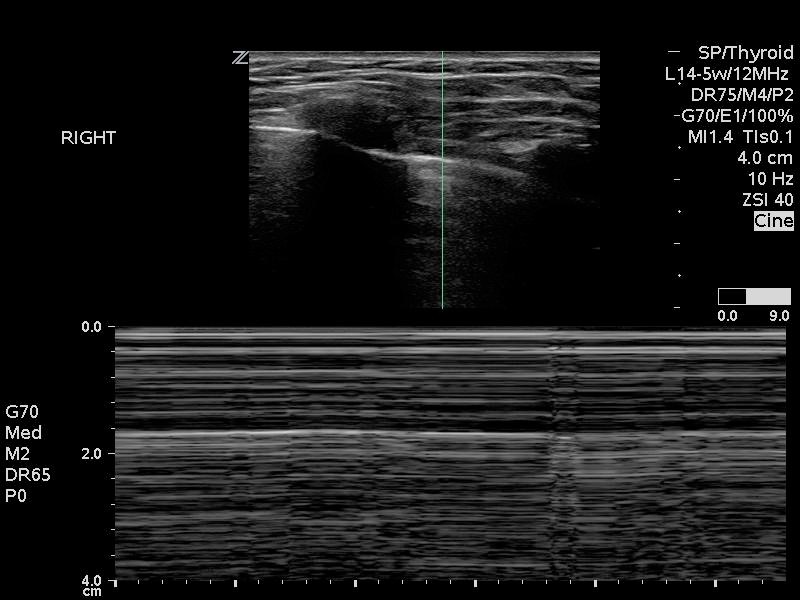
Figure 6: Use of M-mode to identify A) presence (seashore sign) or B) absence (stratosphere sign) of lung sliding
**For more information on lung sliding and lung PoCUS, please revisit the KidSONO Pneumothorax Module**
Tracheal Widening with ETT Cuff Inflation
If the ETT cuff is appropriately placed in the suprasternal notch, distention of the cuff with air can be visualized as widening of the air-filled column on ultrasound (Video 6).
Video 6: Transverse view of widening of the air-filled column due to ETT distention with air
Visualization of a Saline-filled Cuff within the Trachea
Depth can also be evaluated if the ETT cuff is filled with saline, making it directly visible within the airway. Visualization of the saline filled cuff at the suprasternal notch confirms endotracheal intubation whereas non visualization of the cuff signifies endobronchial intubation with a sensitivity of 98.8% specificity 96.4% when compared with fiberoptic bronchoscopy [19]. Position of the ETT cuff above the suprasternal notch in relation to cricoid, subglottic area and tracheal ring can have important implications for tissue damage of the glottic and subglottic structures. Airway POCUS can be used rapidly and accurately in children to determine the depth of the ETT using saline filled cuff [20] (Figure 7).
It is ESSENTIAL to remove the saline once the ETT position is confirmed and reinflate the cuff with air. This limits the possible complication of pressure necrosis with saline filled cuff.
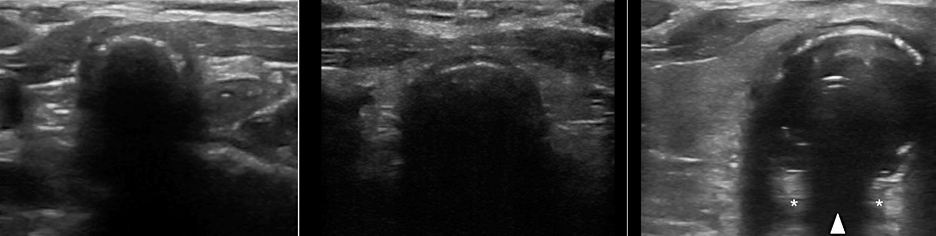
Figure 7. A) Endotracheal vs B) endobronchial vs C) appropriate depth endotracheal intubation intubation using a saline-inflated ETT cuff allowing visualisation of tissues that are posterior to the trachea (*) with saline acting as an acoustic window. Air within the tube results in acoustic shadowing as (white arrowhead), reproduced from Tessaro et al, Resuscitation, 2015 [19]
